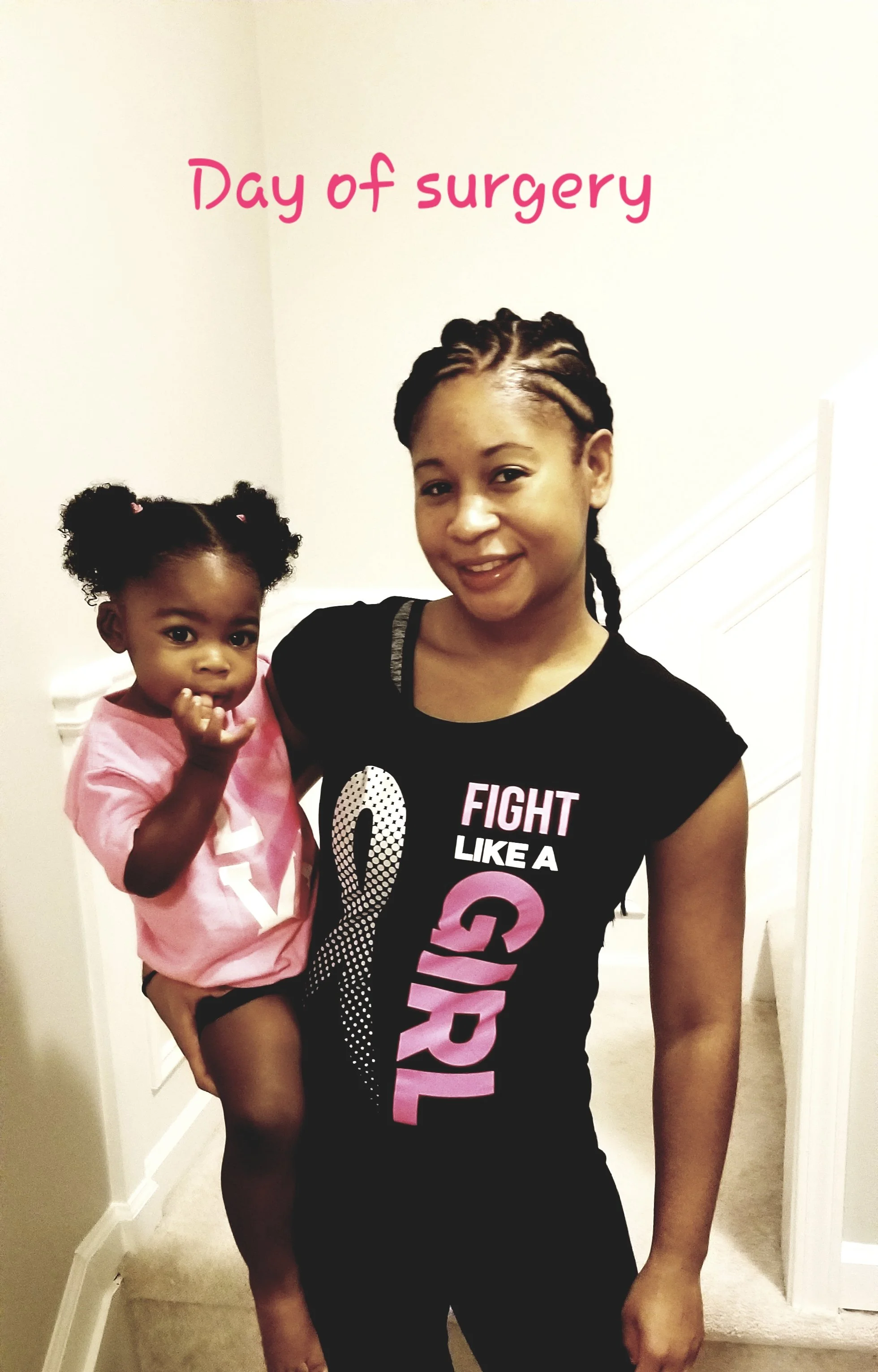She Found TurningPoint as a Breast Cancer Patient. Now She Leads Its Clinical Team.
Written by Melissa Schenkman, MPH, MSJ
A Q&A with Janae Finley, PT, DPT — Early Onset Breast Cancer Survivor & Assistant Clinical Director, Iris Breast Cancer Rehabilitation
Janae Finley, PT, DPT, has lived on both sides of the treatment table. A competitive gymnast turned physical therapist, she was diagnosed with early onset breast cancer in her early 30s — while working in healthcare, while nursing her two-year-old daughter, and before she'd ever heard of anyone her age facing the same diagnosis. Today she's a Doctor of Physical Therapy, a Certified Edema Specialist, and a Certified Lymphedema Therapist, and the Assistant Clinical Director of Iris Breast Cancer Rehabilitation in Atlanta. YMyHealth podcast Co-Host Melissa Schenkman sat down with Janae to talk about her journey from diagnosis to purpose — and everything in between.
What led you to become a physical therapist?
Janae Finley: I've wanted to be a physical therapist since I was probably 13 or 14. I was a competitive gymnast for most of my young life and I was injured — a lot. So I ended up in physical therapy (PT) a lot. In the beginning I hated it, and I hated everyone there. After several more injuries and being in PT for quite a while, I learned to really understand how I could help other athletes. My Olympic dream probably wasn't going to happen, and I thought, this is a great way for me to still do something I love and connect with people.
When I went to physical therapy school, I originally wanted to focus on sports medicine. But after graduating, I actually started in orthopedics — treating little gymnasts, basketball players, back pain, and neck pain. About six and a half years in, I felt like there was something more. Something I could feel more fulfilled by. Iris Breast Cancer Rehabilitation (formerly called TurningPoint) kind of landed in my lap, and here I am, seven years later.
When were you diagnosed, and what did you know about breast cancer in younger women at that point?
I was diagnosed right around the time I hit that six-and-a-half-year mark in orthopedics. And honestly…before my diagnosis, I'd never heard of anyone under 40 with breast cancer. Even with a strong family history — a grandmother, two aunts, another aunt with ovarian cancer, and an uncle with prostate cancer — it just wasn't in my realm of thinking that people were diagnosed this young.
I knew nothing really.
What were your symptoms, and how did you discover something was wrong?
This is a great question, and my patients ask me this a lot. The answer tends to leave them a little jaw-dropped — because I work in healthcare and people think, ‘How did you not know?’
My symptom was bleeding. And like most 30-year-olds, I kind of just ignored it.
I had a benign tumor removed four years before my diagnosis. Then two years after that, I had my daughter, and I had bleeding while nursing. My brain said, ‘It's just related to the tumor, it's the nursing, it's fine.’ I kept telling everyone it was "rusty pipe syndrome" — scar tissue in the duct. I ignored it for probably six to seven months before my husband finally said, “That is not normal.”
He was right.
Here's what I tell people now: Anything that comes out of the nipple should always be milk. Anything other than milk is abnormal, and you should get checked. I didn't even have a lump I could feel. Nothing. Just the bleeding.
What was your reaction when you got the diagnosis?
I was in such shock that I didn't really have much to say. When I told my sister first, she kind of went crazy — crying, questions everywhere. And I just was like, ‘I have no idea.’ I put up a wall. I blocked it out for the first couple of days.
Once I had the biopsy, that's really when it set in. ‘Okay. This is more than I thought. This is serious. This is happening. You've got to get prepared.’
Janae and her then two -year old daughter on the day of Janae’s double mastectomy.
What did your treatment plan look like, and how did you make those decisions?
Initially, I was thought to have Stage 0 — DCIS, ductal carcinoma in situ, where the cancer hasn't spread outside the ducts. But it was so extensive. About seven out of eight ducts in my breast were completely filled with these small calcified tumors. Because of how widespread it was, my doctor told me these three things:
A lumpectomy is not on the table.
A mastectomy was necessary.
The choice of removing one or both breasts was mine.
I thought about it and decided I didn't want to regret anything later. If you're going to take one, you've got to take them both.
I'm glad I made that decision. When I woke up from surgery, I wasn't Stage 0 anymore. I had Stage 1 invasive ductal carcinoma — it had spread outside the ducts. They couldn't see it on the biopsy or imaging; they found it on final pathology. So, going for the double mastectomy was absolutely the right call.
With that staging change, radiation entered the picture. Because I was so young and my family history was so strong, my doctors couldn't pinpoint the cause of my cancer. So they put me on a tumor panel — a board of doctors all reviewed my case. Their analysis and vote came back 50/50. Half said I didn't need radiation; the other half said I did. And then they put the decision all back on me.
I decided: ‘Throw the book at it.’ I went through 28 rounds of radiation to my right breast and chest wall. I didn't need chemotherapy. Then six to nine months after radiation finished, I had the second stage of my reconstruction.
What were the physical and emotional challenges like?
I will be completely honest. I knew what was happening to me physically, but I don't think I emotionally understood what was happening until I got home after my first surgery.
I was so weak from surgery that I couldn't even stand up by myself to take a shower. My husband had to go buy me a shower chair. It's pretty humbling when someone else has to shower you and has to help you use the bathroom. That was the first time I sat and really cried — for a long time — and I just said, ‘Just leave me for a little bit. I need to go through what I'm going through.’
Eventually they started filling my tissue expanders with saline, and I had a little bit of shape again. I did pretty well for a while after that — until I walked past one of those three-panel mirrors in a store dressing room and saw everything at once: incisions on my breast, a large incision on my back from reconstruction. All at the same time.
That was emotional too.
But I've worked through it. Now I'm at the point where I'm like, I don't care. Battle scars. Everyone's got scars in life, and it is what it is.
Janae ringing the bell marking completion of her 28 rounds of radiation.
What helped you cope emotionally?
Before I came to TurningPoint (now Iris Breast Cancer Rehabilitation), I had nothing. No options. TurningPoint is really what gave me resources — and made it okay to consider counseling. I had never been to a counselor prior to my diagnosis.
Coming into a diagnosis this life-changing, you feel like no one is really going to understand you. But it was the best decision I could have ever made. I still see a counselor. I still check in with her.
To know that someone emotionally understands where you are, can meet you at that level, and can help you find real ways to cope — not just ‘take a deep breath and keep moving’ — that changed things for me. I continue to learn new ways to cope each year, each month.
Some of the other things that have made a real difference:
Sound baths — I was confused at first (‘What is this lady doing with these bowls?’), but mindfulness and sound baths have become my favorite thing. If you've never experienced one, try it.
Yoga — Not only did it help me physically improve my flexibility post-radiation, it became a way to relax and live in the moment. It gave my mind somewhere else to go.
Counseling through TurningPoint (*now Iris Breast Cancer Rehabilitation)— Both of our current counselors are breast cancer survivors themselves. That connection is something you just can't get anywhere else.
How did you end up at Iris Breast Cancer Rehabilitation (formerly TurningPoint) as a clinician?
When I was diagnosed, the assumption — because I'm already a PT — was that I'd be fine and didn't really need anything. You can figure it out. But I came to them saying, I can't even lift my arm to my shoulder, and I have a two-year-old. That's when someone said, let us send you to Turning Point (*now Iris Breast Cancer Rehabilitation). And I thought, ‘What's a TurningPoint ? Why haven't I heard of it?’
I looked them up and instantly thought, ‘Where has this been my whole life?’
When I stepped through the doors the first time, a calm just came over me. It felt like home. It's a mix between a spa and physical therapy — low lighting, one-on-one treatment, homey and down to earth and very personable. I came in for my third PT session and my therapist asked if I'd thought about working there. I said okay.
She said, ‘We're going to finish up your PT, you'll get through the rest of your treatments, and I'll see you in a few months as your coworker.’
That experience changed my whole outlook on why I was diagnosed. You go through that why — and no one could tell me why. I went down a rabbit hole for a while, thinking maybe it was something I had done. But now I look at it as a ‘Why not me?’ diagnosis. It wouldn't have gotten me where I am today if it hadn't happened.
What makes Iris Breast Cancer Rehabilitation (*Formerly TurningPoint) unique?
We're one of the only nonprofits in the U.S. — and especially in the South — that does what we do and has all of these services together in one place. Our founder wanted to make sure that no one was turned away regardless of ability to pay and that all the services a patient might need during their journey are available under one roof.
So, you're not going across town for one thing and across town again for another. You can get it all in one place, with a team that all knows each other and knows you. Services include:
Physical therapy (the core of what we do)
Massage therapy
Counseling (with counselors who are breast cancer survivors themselves)
Nutritionist referrals
Exercise classes and educational events
First Friday Flow — a gentle, calm stretching session on the first Friday of every month
How do you help patients with pain and body image in your work?
Pain is one of the biggest things patients come in with. The therapies we recommend and do with each patient really depend on the type of pain. Patient presentations and needs include:
Hypersensitivity- Some patients after surgery are hypersensitive. So, we desensitize those areas using very gentle stimuli and essentially retrain the brain through sensory normalization — telling the body, ‘This does not hurt.’
Lack of Movement- Some patients just need to move again. After surgery, they're told not to raise their arms above shoulder level, and they take it completely literally. They come in walking around with T-Rex arms six to eight weeks later. Movement itself can dramatically reduce pain, and nobody told them it was okay to move again.
Challenges to Body Image- Some patients don't want to look in the mirror for several sessions. We might have them start by standing sideways so the mirror is in their peripheral vision — just a glimpse. Then 30 seconds facing the mirror once a day. Gradual, gentle reintroduction to what they see. And sometimes it's just reassurance that it's okay — that they're allowed to touch the area, that it won't hurt anything.
For body image, we take it gradually. Sometimes we're the first people who've seen their results alongside them.
What would you say to a young woman just diagnosed?
You have to be your own advocate. I was lucky to have a great team, but not everyone is. You have to make your voice heard — tell people what you need, what you want, ask every question you have. Make the doctor stay in the room until you're done. Because if you don't ask, you're never going to get the answer.
And I would tell them: it's not a death sentence. Breast cancer — whether it's Stage 0 or Stage 4 — used to be very hush-hush, very unknown. But it's such a survivable, treatable cancer. There is life after treatment. There is life after chemo. There is life after radiation. If you have goals, they may be on pause. But once you're done, keep working toward them. You'll get there — maybe not the same way you imagined, but you'll get there.
What do you wish people who haven't had cancer understood?
Don't be afraid to talk to us. Don't be afraid to ask questions. We're not china in a cabinet — you're not going to break us. We are people just like everyone else. Life may look a little different for us, but we can get there too.
And communicate with each other. If someone you know is diagnosed, have the conversation. Show up. We'll give you the answers.
Janae and her young family.
If you could go back and tell your pre-diagnosis self one thing, what would it be?
A couple of things, actually.
First: Take a deep breath. I kept things in for so long. I put on a happy face like everything was great when it wasn't. I would tell myself: it's okay to not be okay. That is normal right now. You've got to talk about it, or it's going to drive you crazy.
Second: There's a light at the end of the tunnel. You won't understand it at first. But in hindsight, you are really going to understand why this happened.
And I do. I really do.
How can people connect with you and Iris Breast Cancer Rehabilitation?
You can visit the Iris Breast Cancer Rehabilitation (*Formerly Turning Point Breast Cancer Rehabilitation) website here. Iris is a nonprofit organization in Atlanta serving breast cancer patients and survivors. To support their mission, look out for the annual Strides for Survivors walk and the Pink Affair gala.
Want to hear more from Breast Cancer Survivor and Physical Therapist, Janae? Check out the YMyHealth Podcast on our YouTube channel or on your favorite streaming platform!